Intermittent Fasting and GLP-1 for Metabolic Disorders
Metabolic disorders, such as obesity and insulin resistance, have become a major health concern worldwide. Researchers have been exploring various strategies to manage these conditions, including intermittent fasting (IF) and glucagon-like peptide-1 (GLP-1) medications. This narrative review focuses on the effects of IF and postprandial GLP-1 secretion in individuals with different metabolic conditions and degrees of glucose intolerance.
Benefits of Intermittent Fasting
Intermittent fasting has been shown to improve insulin sensitivity, reduce inflammation, and enhance fat oxidation, leading to weight loss and improved metabolic health. Various studies have reported the benefits of IF, including improved glucose tolerance, reduced body fat, and increased human growth hormone (HGH) production.
GLP-1 Medications: A Powerful Tool for Metabolic Management
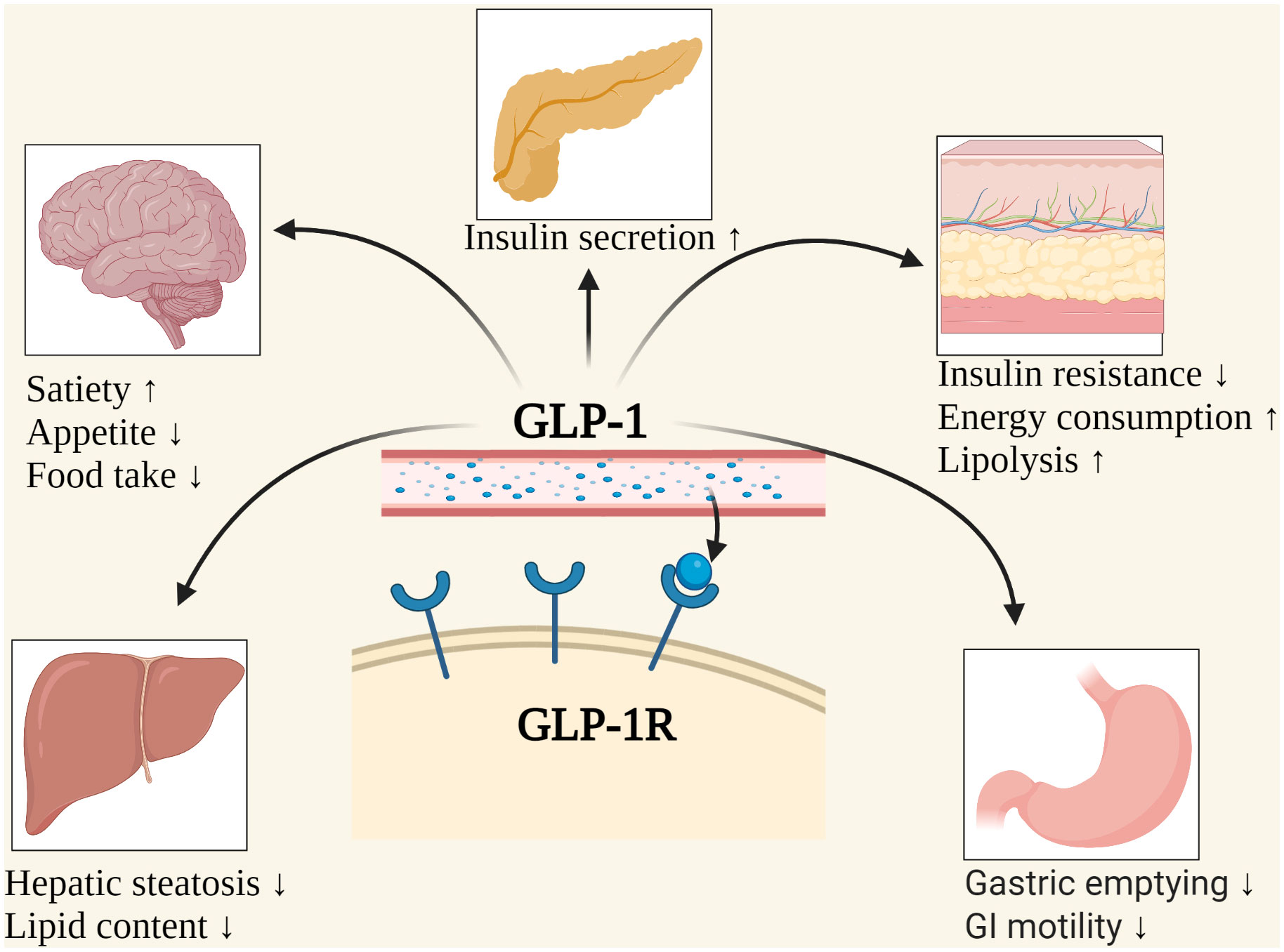
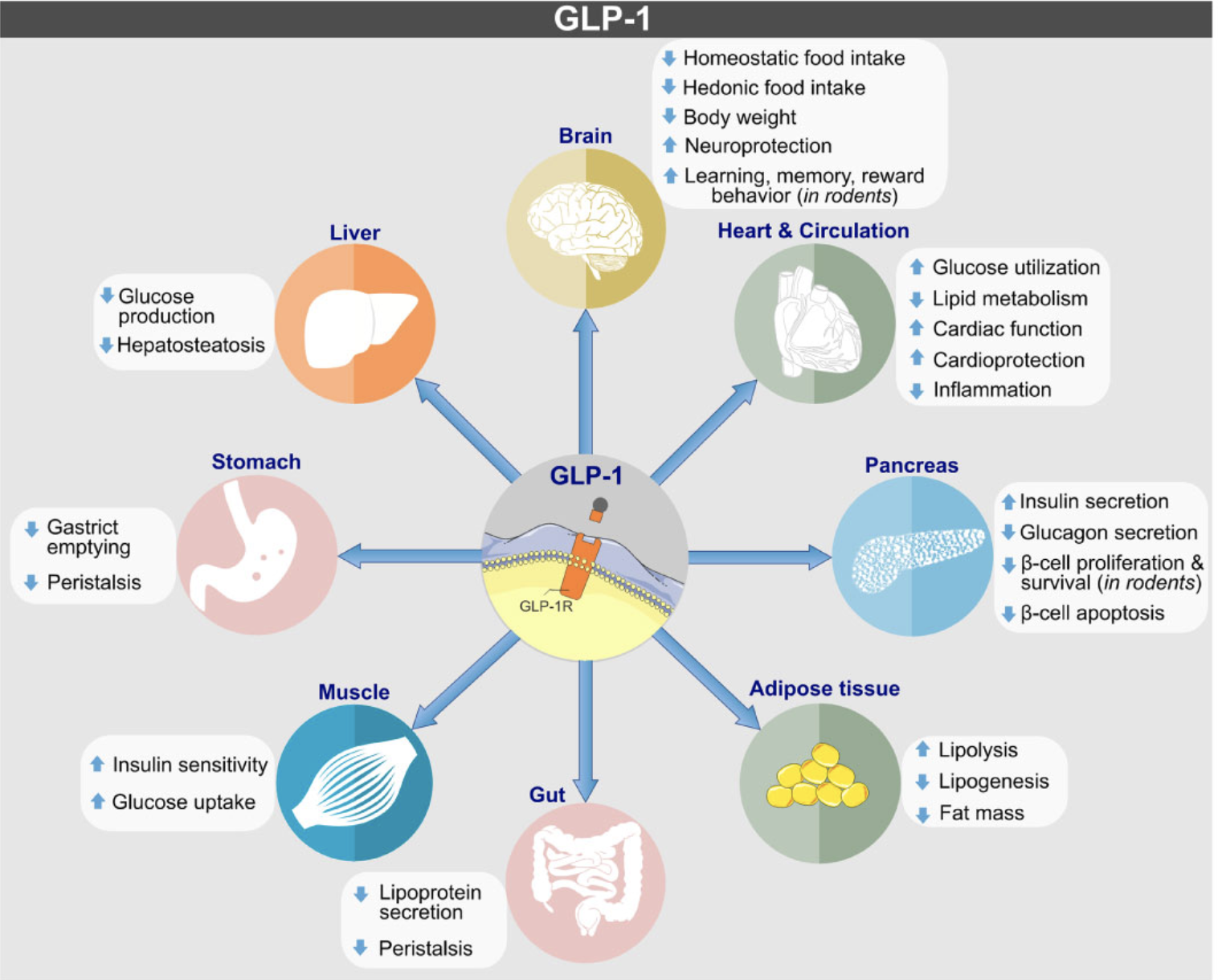
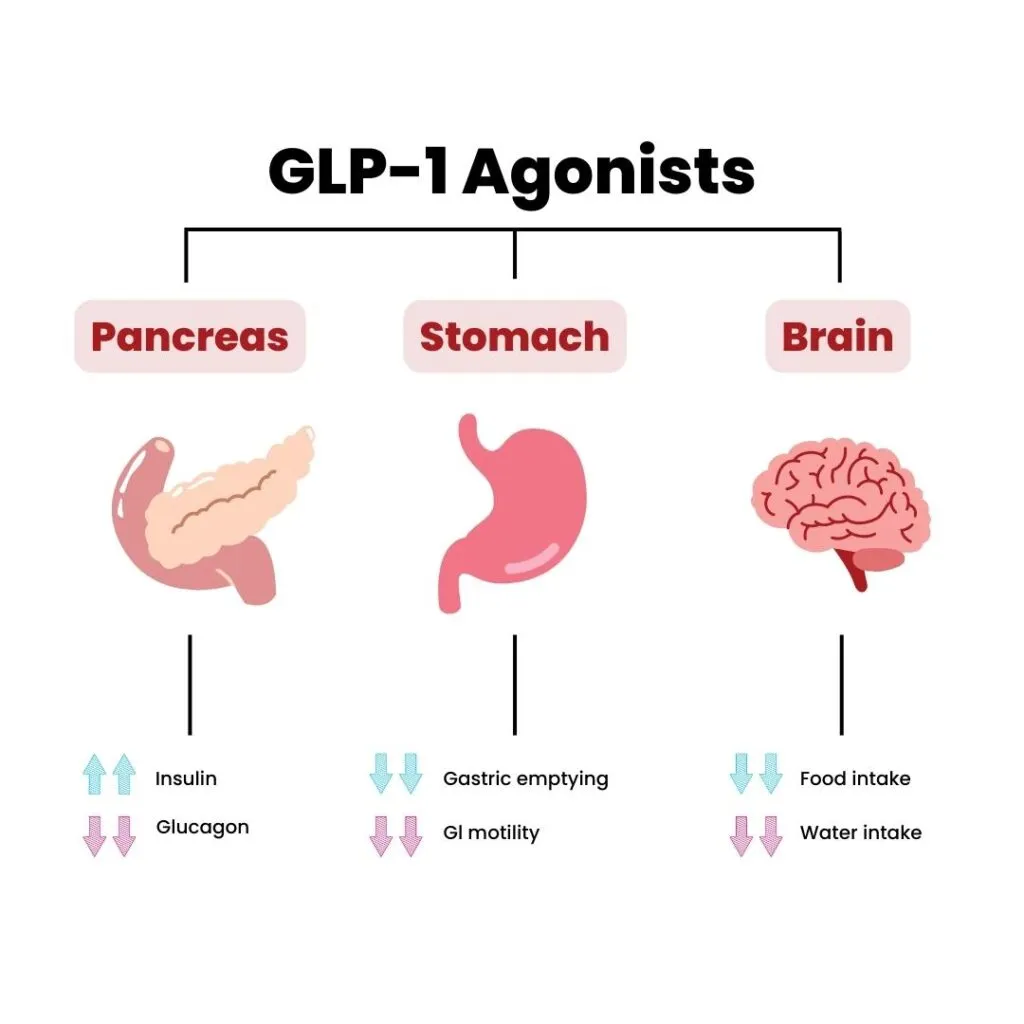
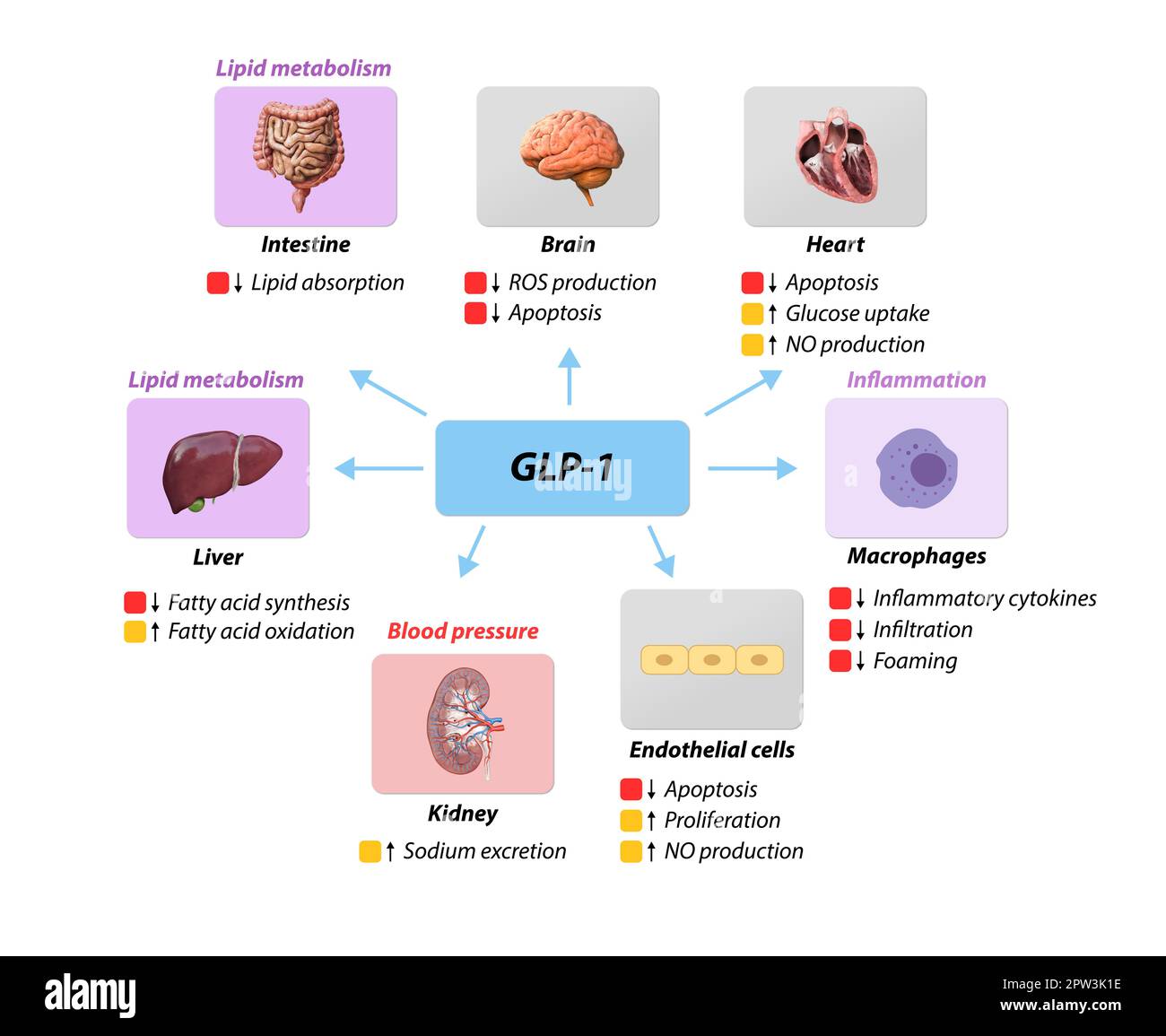
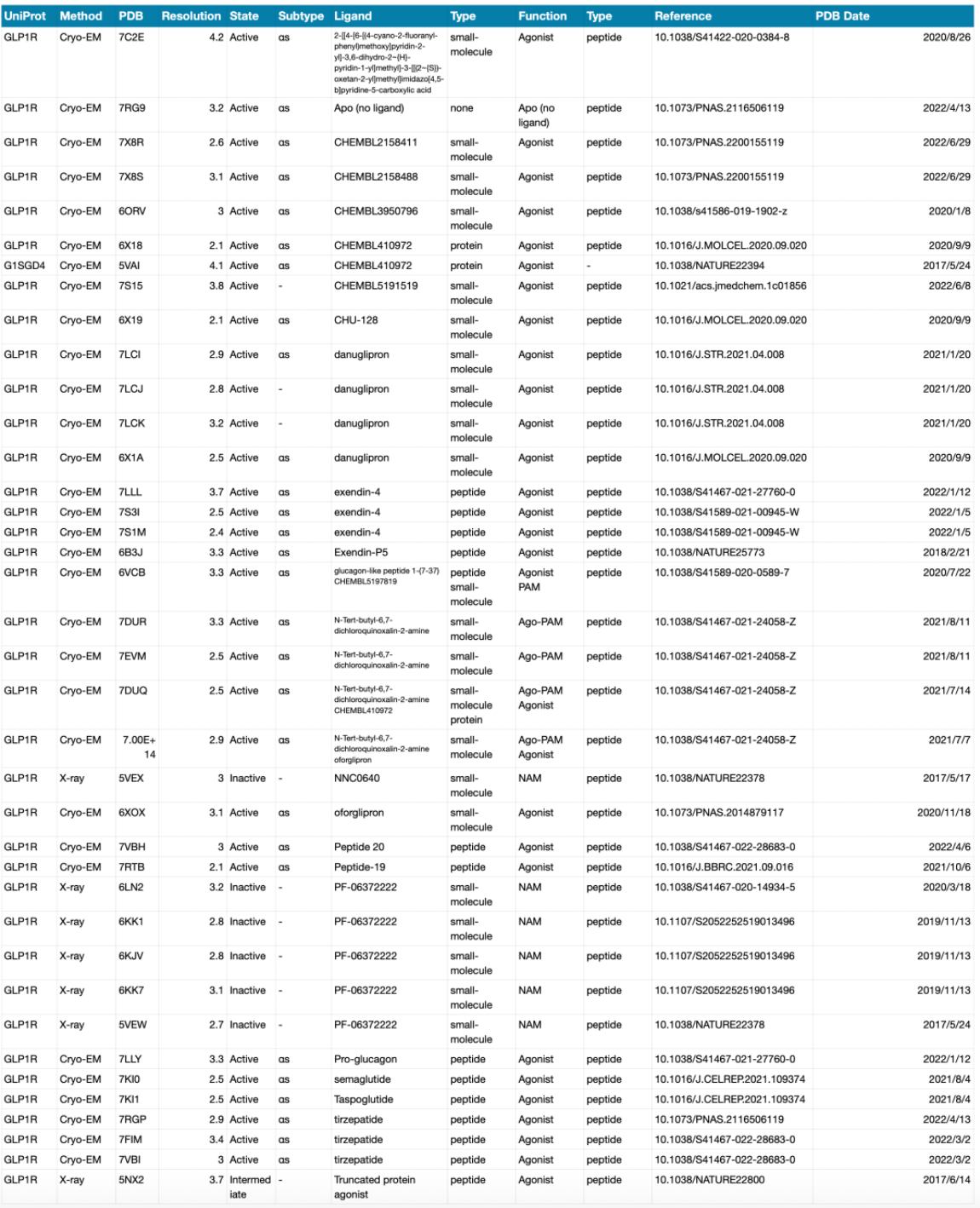
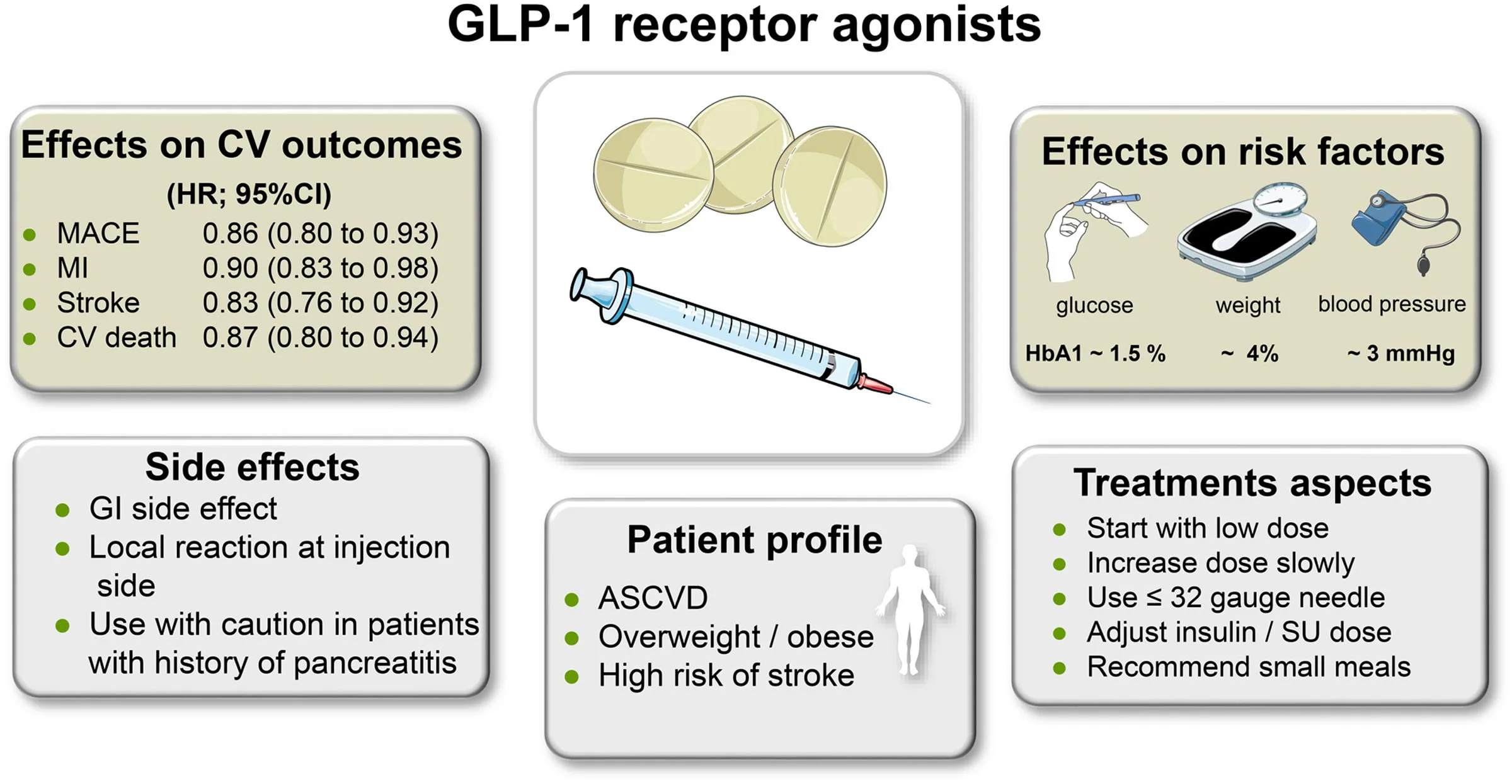
GLP-1 medications, such as semaglutide (Ozempic) and liraglutide (Saxenda), have revolutionized the treatment of type 2 diabetes and obesity. These medications work by mimicking the action of GLP-1, a hormone that regulates appetite and blood sugar levels. By suppressing appetite and delaying gastric emptying, GLP-1 medications lead to significant weight loss and improved glycemic control.
The Relationship Between Intermittent Fasting and GLP-1
Research has shown that combining IF with GLP-1 medications can be a potent strategy for accelerating weight loss and improving metabolic health. A study published in the Journal of Clinical Endocrinology and Metabolism found that individuals who followed an IF regimen (12:12) and received GLP-1 medication (semaglutide) experienced greater weight loss and improved insulin sensitivity compared to those who received medication alone.