Energy Autonomy and GLP-1 Protein Secretion Responses
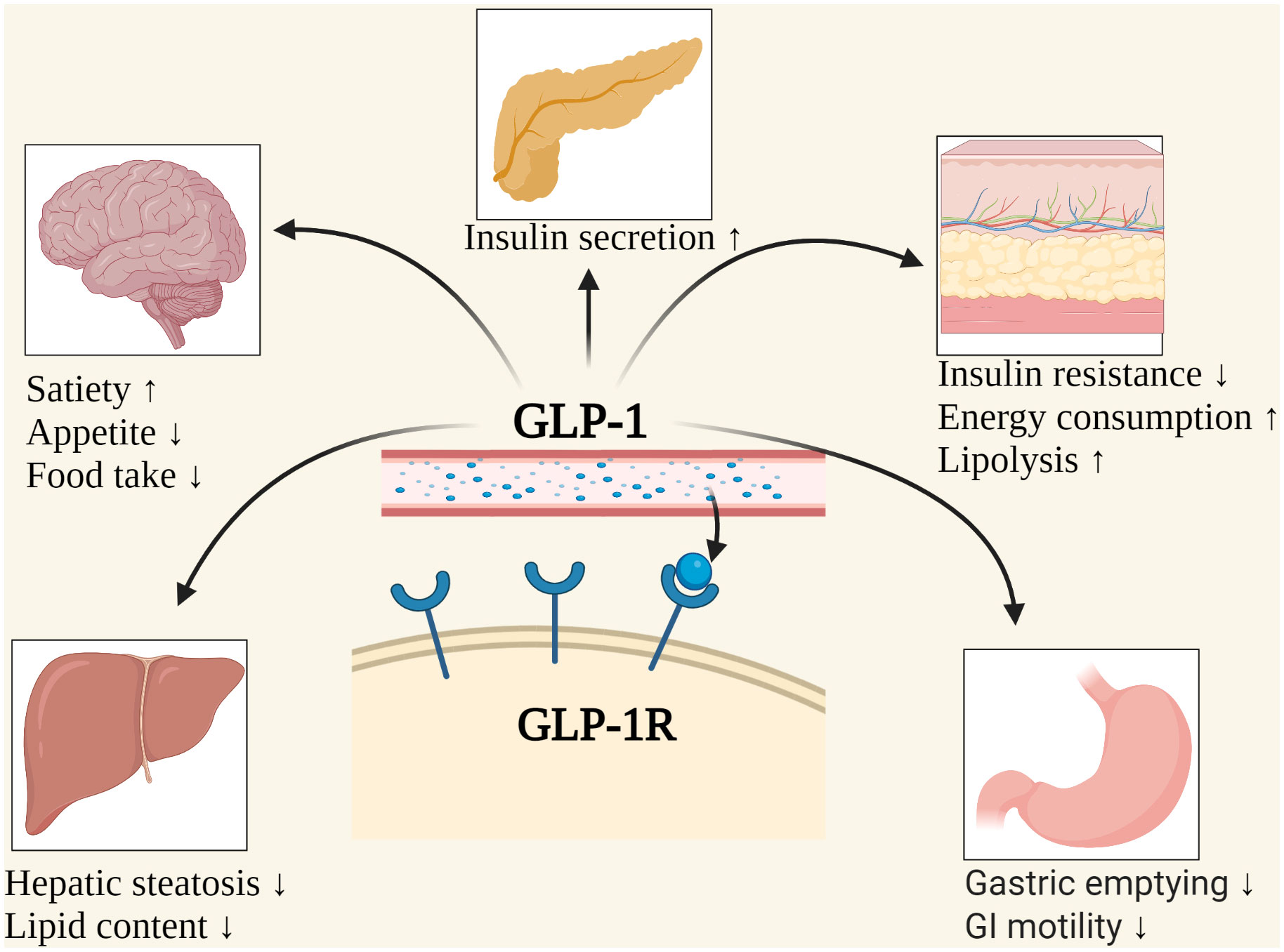
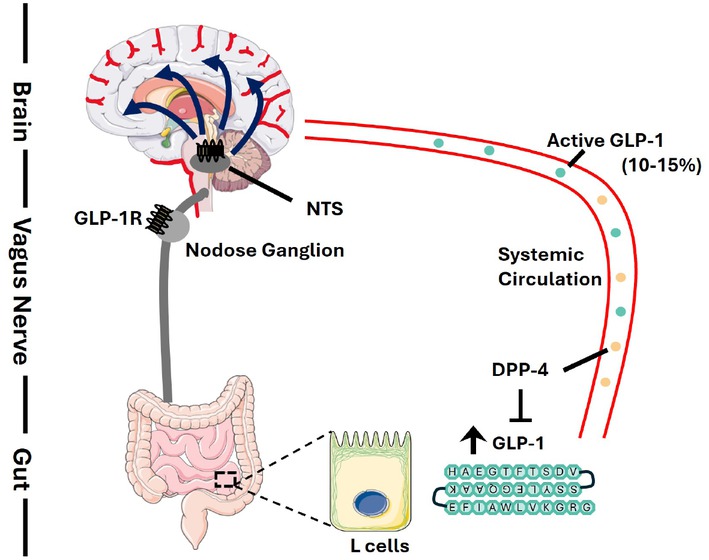
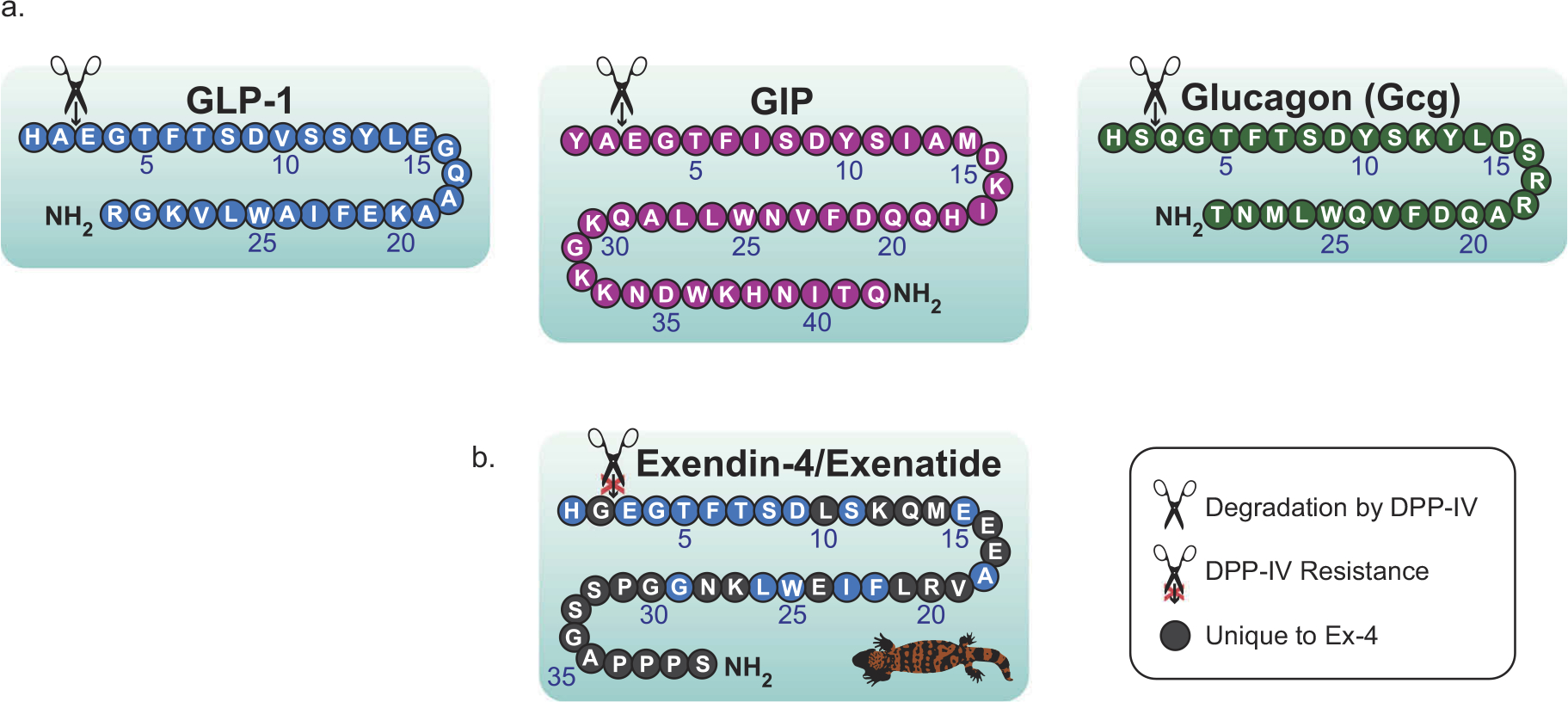
The intricate relationship between energy autonomy and glucagon-like peptide-1 (GLP-1) protein secretion responses has garnered significant attention in recent years. GLP-1 is an incretin hormone produced in the intestine, secreted in response to nutrient exposure, and plays a pivotal role in glucose metabolism, insulin secretion, and appetite regulation.
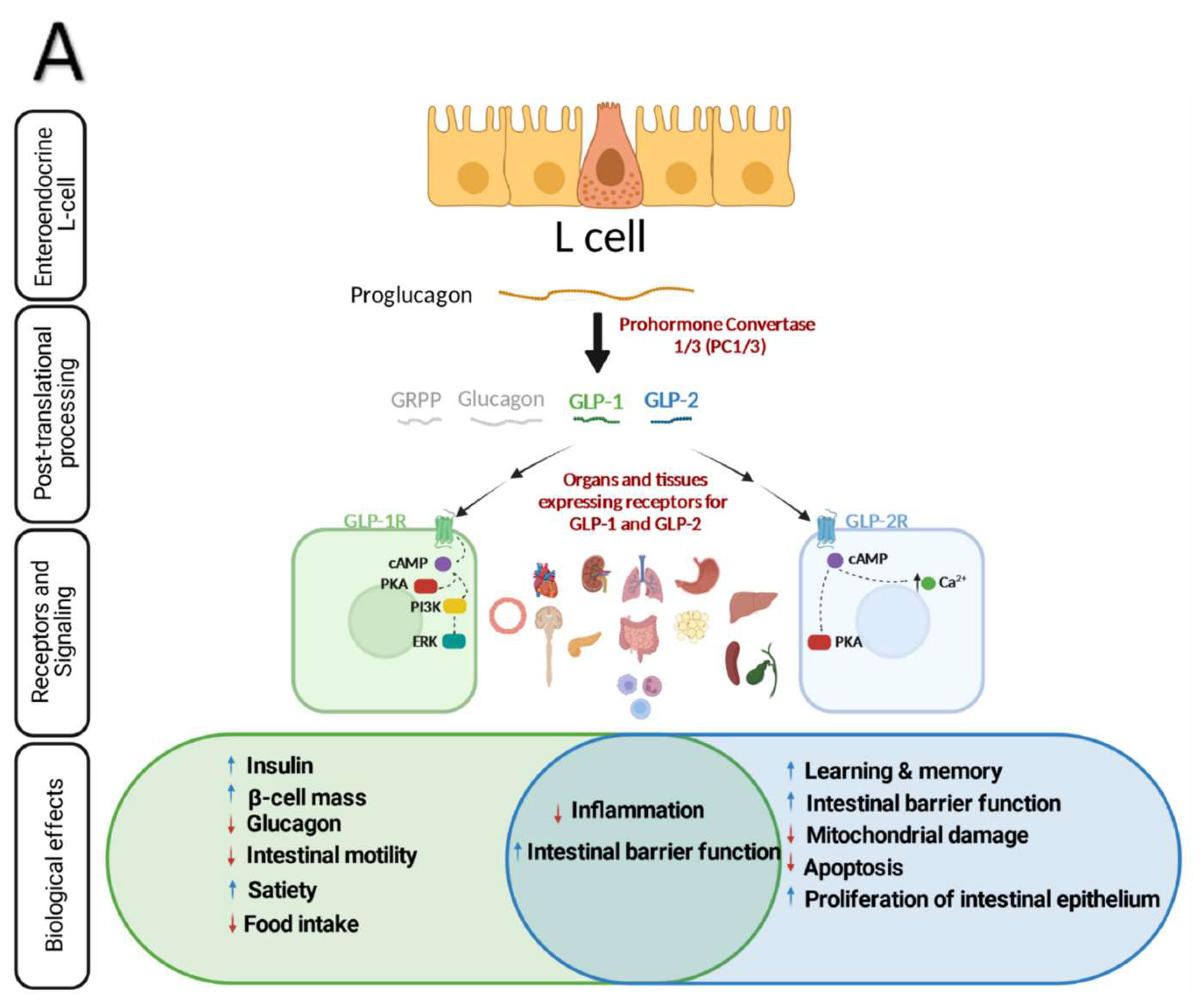
The Mechanism of GLP-1 Secretion
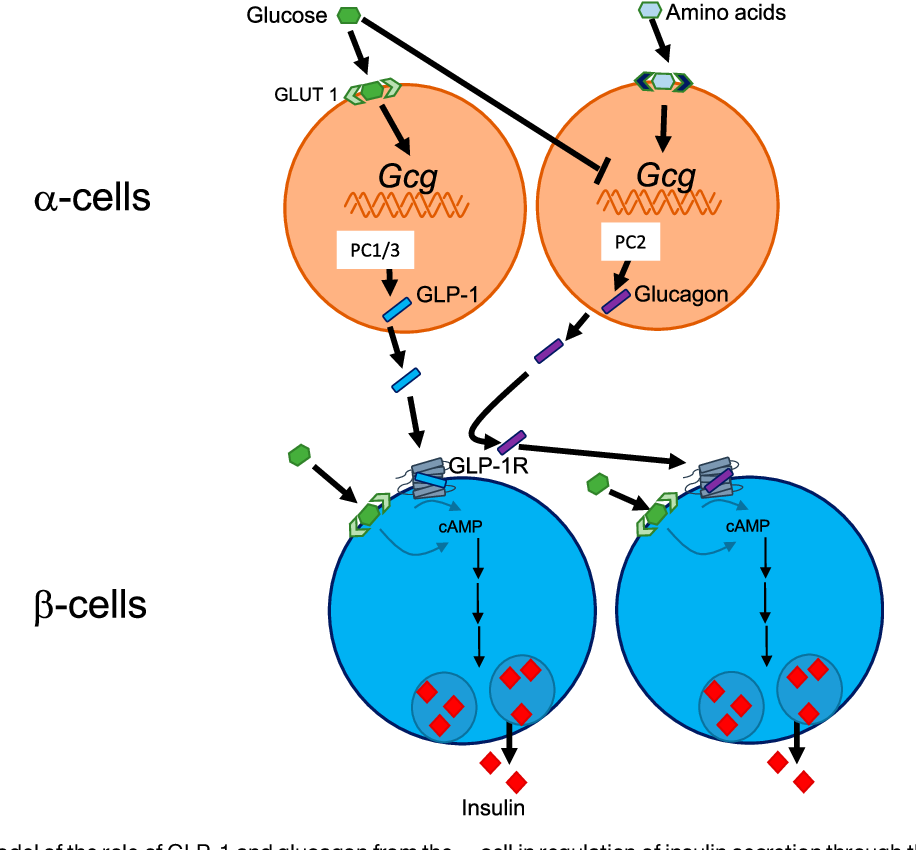
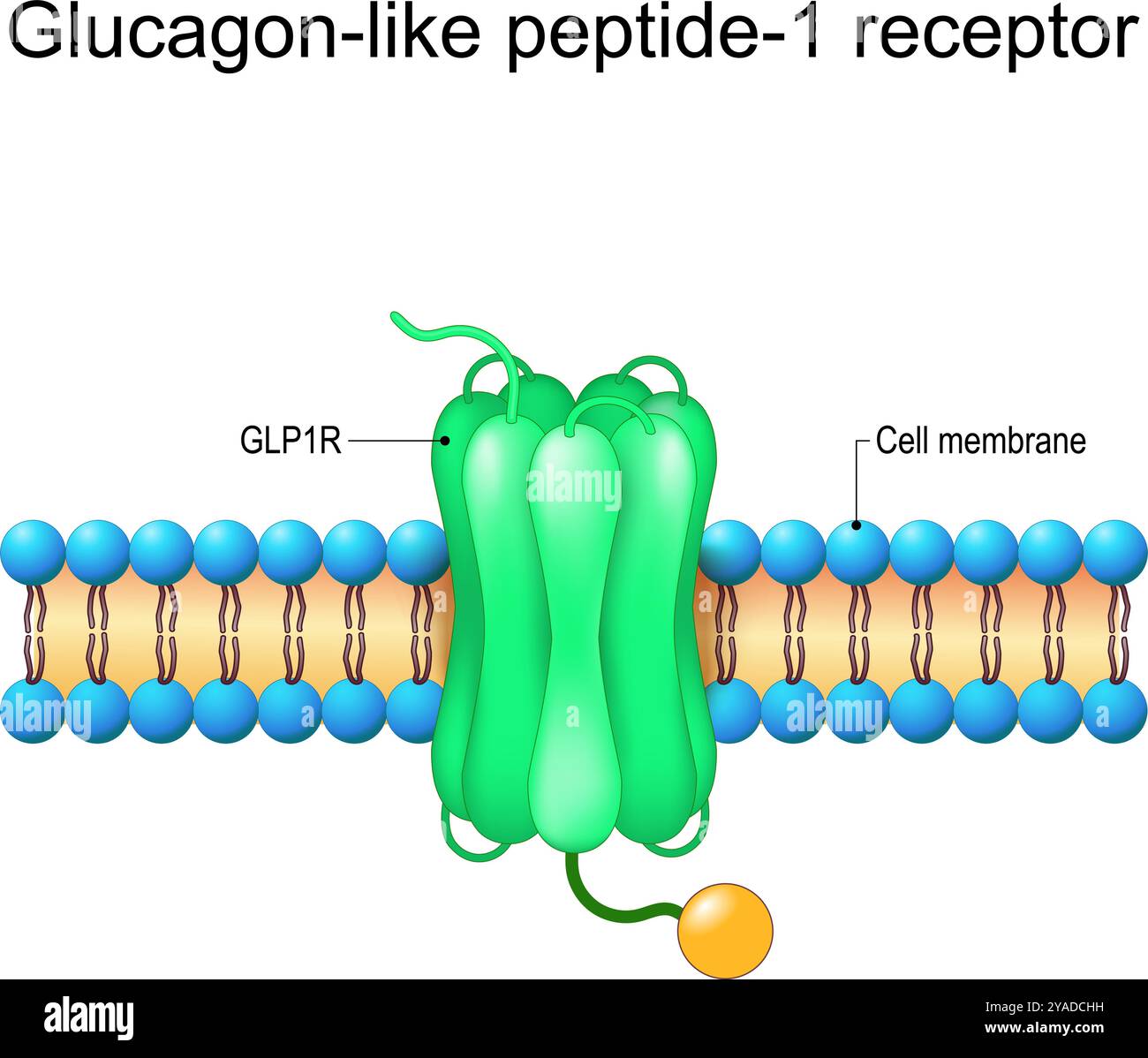
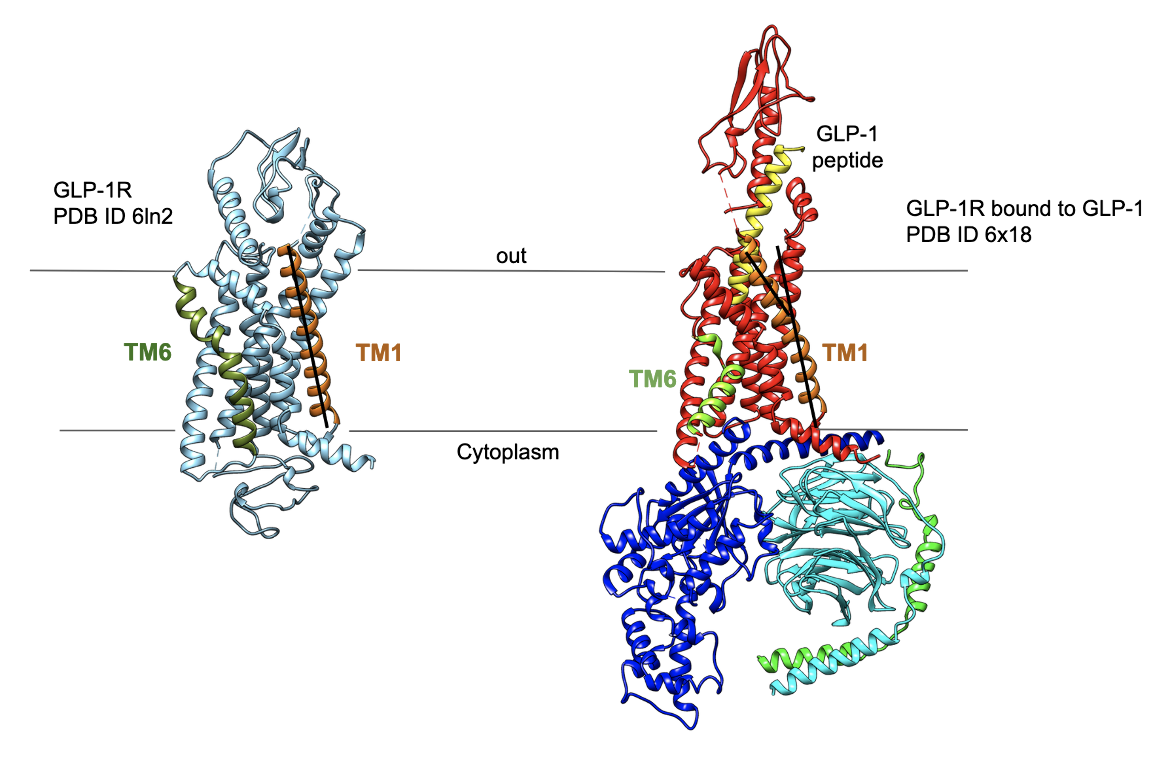
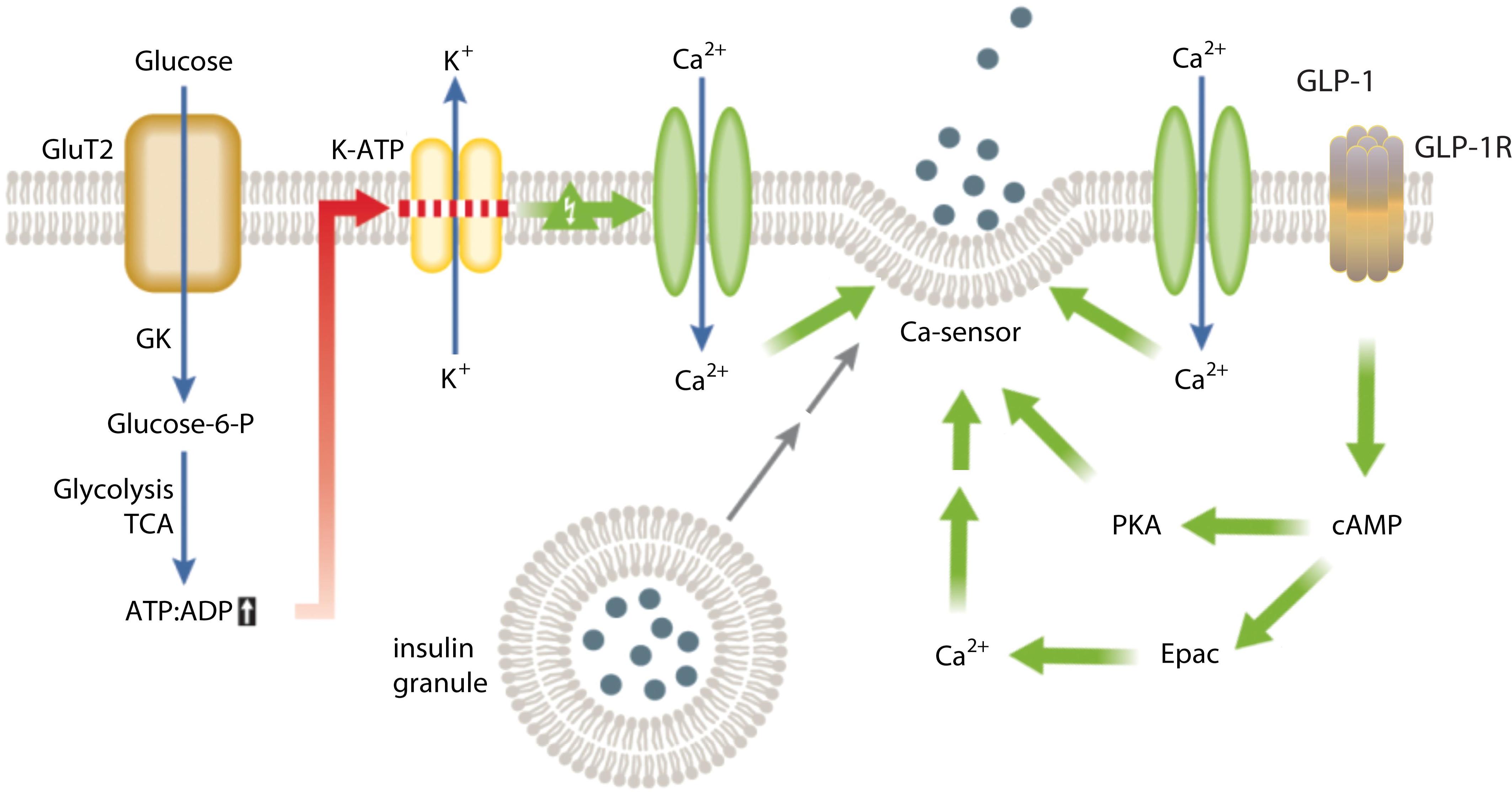
GLP-1 secretion is triggered by the presence of nutrients, such as glucose, fat, and amino acids, in the gut. This hormone potentiates insulin secretion from pancreatic β-cells and promotes satiety. The mechanisms underlying GLP-1 secretion and clearance involve a complex interplay of transporters, G-protein-coupled receptors, and signaling pathways.
Energy Autonomy and GLP-1 Secretion

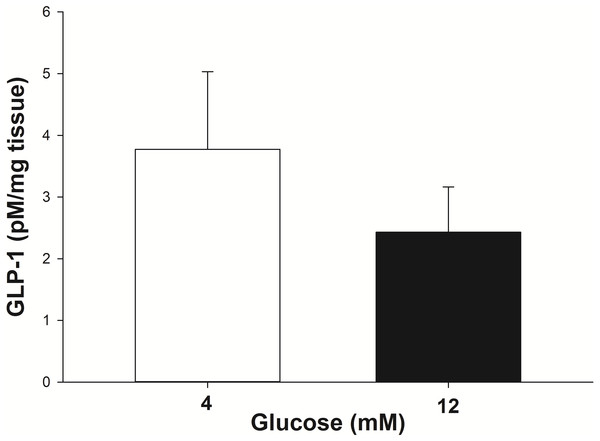
Energy autonomy refers to the body's ability to regulate its energy balance, comprising energy intake, energy expenditure, and energy storage. GLP-1 plays a crucial role in maintaining energy homeostasis, and its secretion is influenced by various factors, including nutrient availability, energy status, and body weight. Studies have shown that GLP-1 secretion is lower in adults with obesity or type 2 diabetes mellitus, suggesting a possible link between GLP-1 dysregulation and metabolic disorders.
GLP-1 Signaling and Energy Expenditure
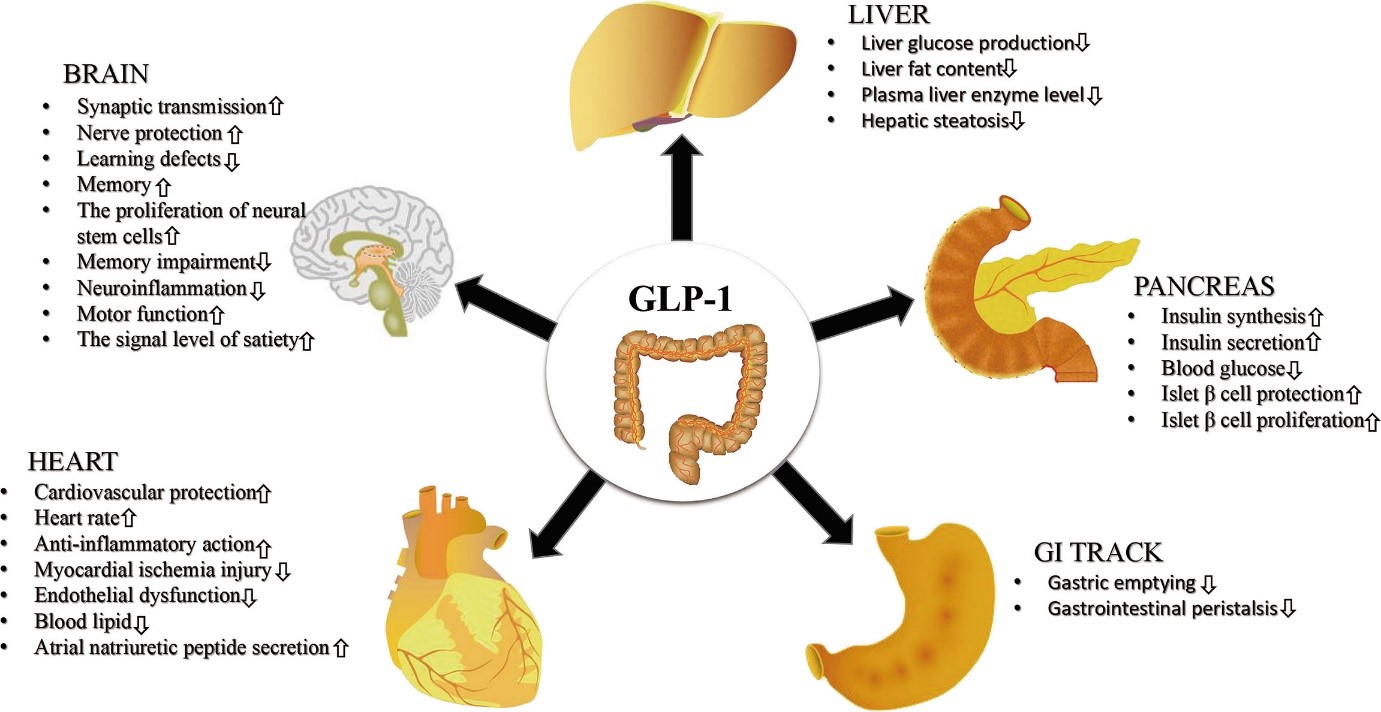
GLP-1 signaling pathways modulate energy expenditure in various tissues, including the pancreas, liver, skeletal muscle, and adipose tissue. In the pancreas, GLP-1 enhances insulin secretion and beta-cell function, while in the liver, it stimulates glucose output and glycogen synthesis. In skeletal muscle, GLP-1 promotes glucose uptake and glycogen synthesis, while in adipose tissue, it regulates lipolysis and fatty acid oxidation.